Sebaceous
adenitis in rabbits
Esther van
Praag, Ph.D.
|
MediRabbit.com is
funded solely by the generosity of donors. Every
donation, no matter what the size, is appreciated and will aid in the
continuing research of medical care and health of rabbits. Thank you |
Warning: this
file contains pictures that may be distressing to some persons
|
The etiology of sebaceous adenitis – also called inflammation
of the sebaceous glands - is not well understood; it is considered
idiopathic, inherited or endocrine. In rabbits, the disorder appears to have
an inherited autoimmune origin, accompanied by a defect of the fatty acids
metabolism. An autoimmune origin also established in dogs, after
immunohistological analysis of skin samples, but also from the successful
treatment with cyclosporine, an immunosuppressant drug. Clinical characteristics The
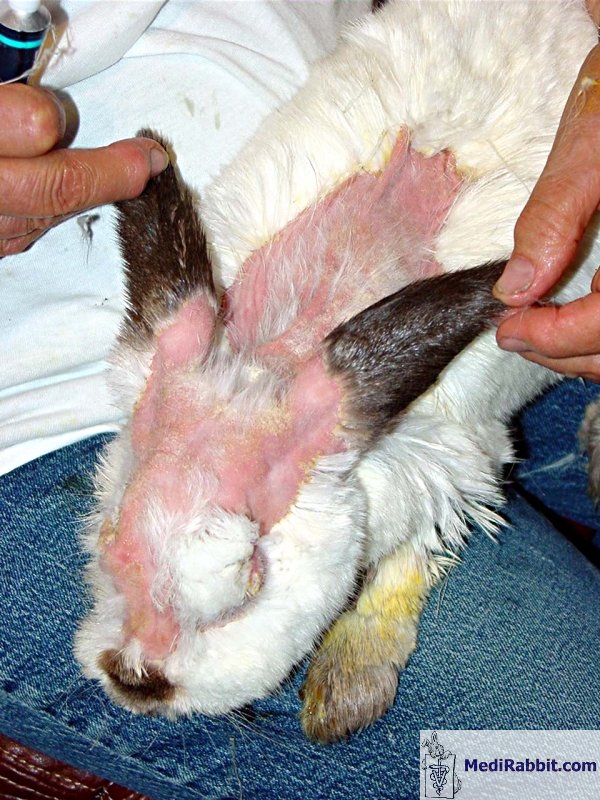
first clinical manifestations of sebaceous adenitis resemble those of skin
allergy: inflamed sebaceous gland with progressive destruction of the glands
and the adjacent hair follicles, accompanied by inflammation of the hair
follicles (mural lymphocytic folliculitis). The condition worsens over time.
Hair growth stops, the fur is thinning, and alopecic patches appear. The skin
becomes erythematous, with abnormal thickening (hyperkeratosis). Scales
adhere tightly to the skin. Infiltration of lymphocytes into the basal layer
of the epidermis (interface dermatitis) is furthermore observed in rabbits.
This causes changes in the basal cells of that layer, necrosis of
keratinocytes and occasionally inflammation of the follicular-dermal
interface (interface folliculitis). Sebaceous
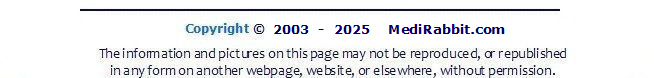
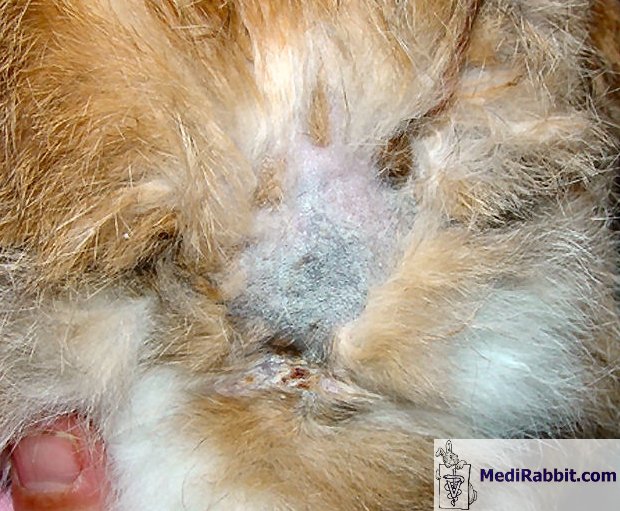
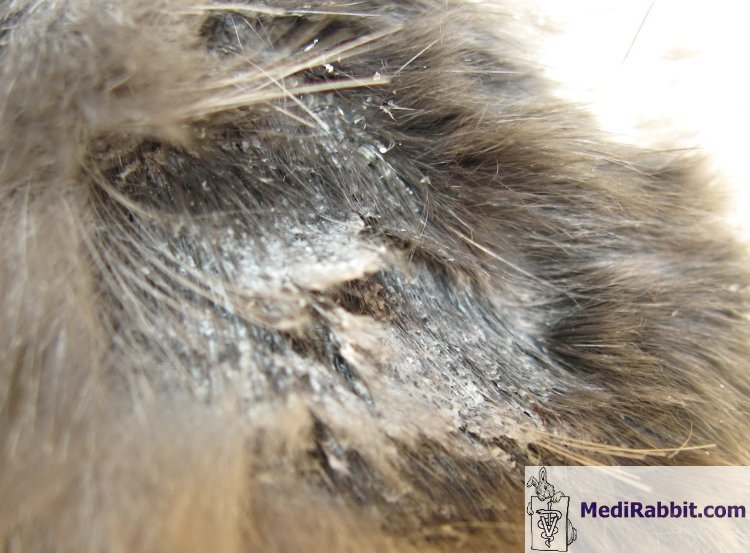
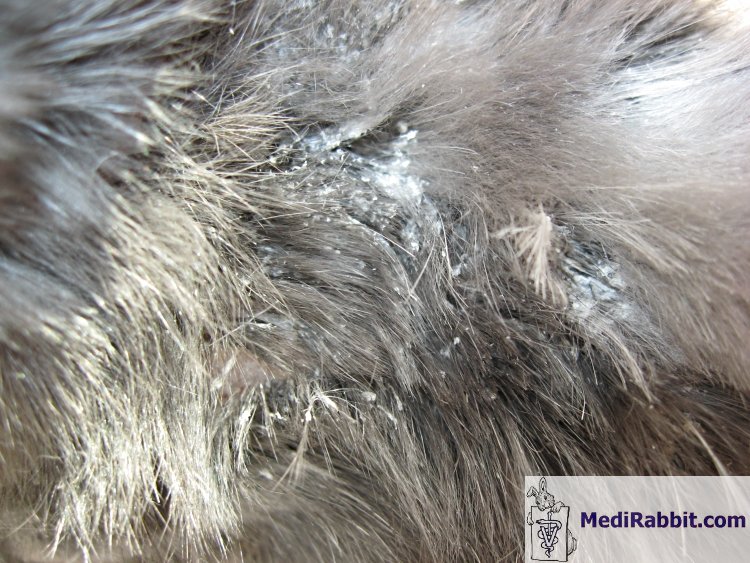
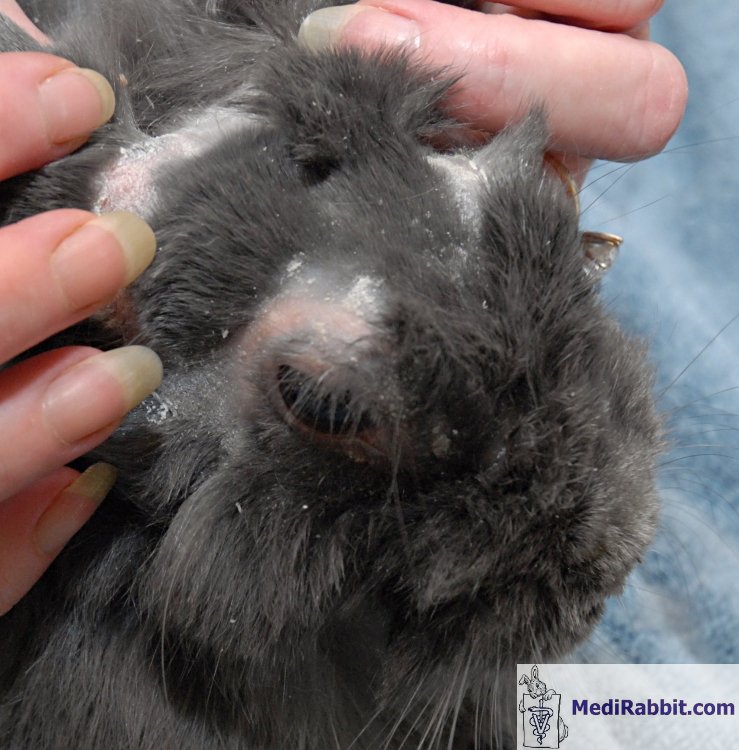
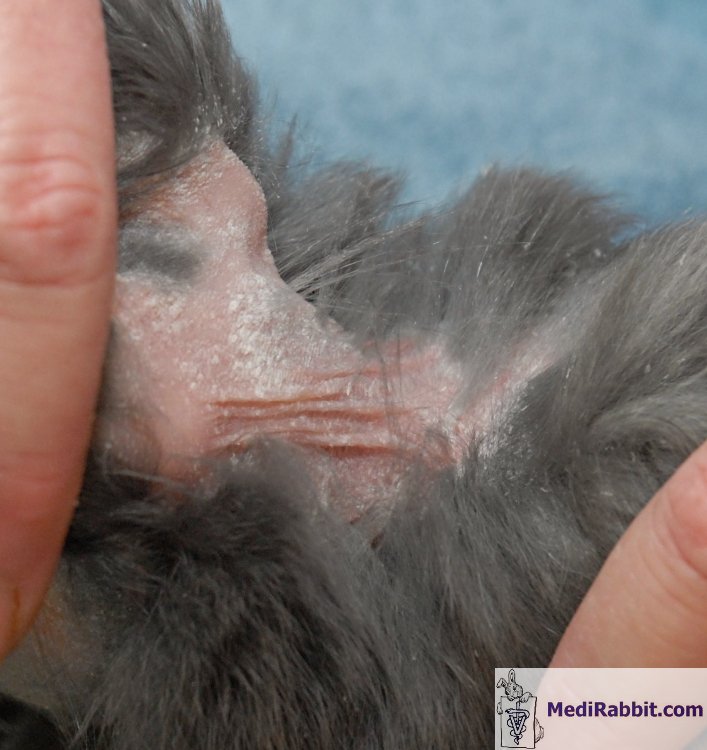
adenitis in rabbits can occur in patches or be progressive, with non-pruritic
scaling on the head. It later spreads to the neck, the pelvic region, and the
rest of the body. Lesions are often symmetrical over the head and abdomen.
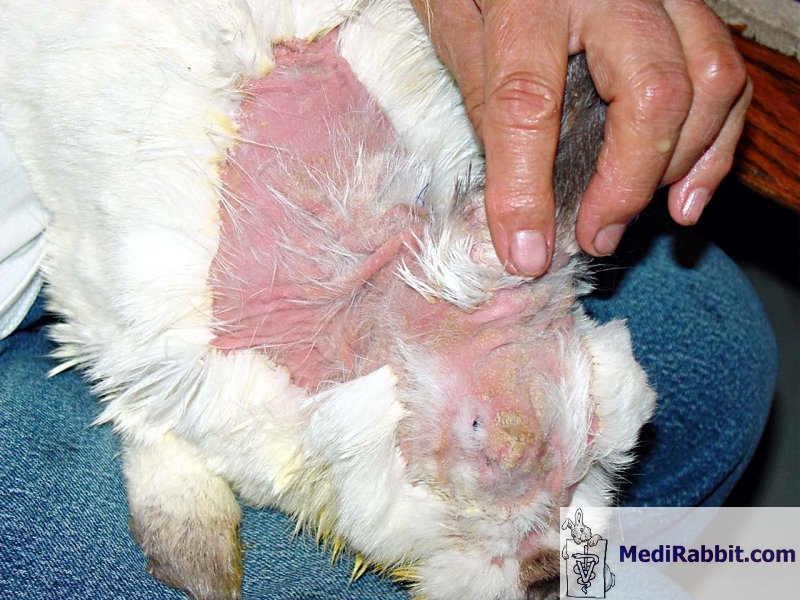
Sarah Davoli Coco, older rabbit
suffering from confirmed patchy sebaceous adenitis in the pelvic region. Diagnosis Inflammation
of the sebaceous glands is often mistakenly diagnosed as skin allergy. As a
result, it is treated inappropriately. Skin problems such as fungal dermatitis,
parasitic infestation or defluxion will often be considered, when the
proposed skin allergy treatment fails to bring an improvement. This skin
condition should furthermore be differentiated from thymoma-associated exfoliative dermatitis, cutaneous lymphoma, or dermatitis
caused by autoimmune hepatitis. To
avoid unnecessary distress of the rabbit, it is important to do a biopsy of the
skin, and have it analyzed by a pathologist with knowledge of rabbit tissue
specificities. Radiography of the chest helps rule out thymoma. Treatment There
is no treatment for sebaceous gland inflammation, except good care. In dogs,
this problem is treated by cleaning the skin with a detergent soap twice a
week/month, clean its skin, followed by an
application of a chlorhexiderm solution, and baby oil. This helps loosen the
skin dandruff and provides the necessary fat to the skin. A
regular brushing also helps to remove the dandruff, which is a source of
secondary bacterial infection. Treatments with an antifungal,
corticosteroid or an immunosuppressant drug did not bring improvement. The
administration of fatty acids, vitamin A or retinoids (e.g. isotretinoin,
etretinate) can be attempted, but the toxicity of these compounds must be
taken into account. The combined administration of
cyclosporine (5 mg/kg, PO, sid), medium chain triglycerides and essential
fatty acids, accompanied by topical application of propylene glycol (spray)
was successful in the treatment of sebaceous
adenitis in a rabbit. Two months later, remission was observed, with new
hair growth. Since this
treatment is costly, euthanasia should be considered as a humane alternative,
so as not to unnecessarily prolong the rabbit's pain
and suffering. If secondary bacterial infections develop, it should
be treated with appropriate antibiotics and/or an antiseptic cream.
For detailed information on sebaceous adenitis in
rabbits, see: “Skin Diseases of Rabbits”, by E. van Praag, A. Maurer and T.
Saarony 408
pages, 2010. Acknowledgements A
special thanks to Sarah Davoli, Lyne Lavigneur, Nancy LaRoche, Nancy Martin
and Debbie Hanson for sharing the pictures of their rabbits Coco, Lulu,
Jenny, and Bella, suffering from sebaceous adenitis.
Further reading Florizoone K. Thymoma-associated
exfoliative dermatitis in a rabbit. Vet Dermatol 2005;16:281-284. Jassies - Van
der Lee A, van Zeeland Y, Kik M, Schoemaker N. Successful treatment of
sebaceous adenitis in a rabbit with ciclosporin and triglycerides Vet
Dermatol 2009;20:67-71.
Marcel Kovalik, Keith L. Thoday, Kevin Eatwell, and Adri H. M. van den Broek. Successful treatment of idiopathic sebaceous adenitis in a lionhead rabbit. Journal of Exotic Pet Medicin 2012; 21: 336–342. Quesenberry
KE, Carpenter JW. Ferrets, rabbits and rodents. Clinical Medicine and
Surgery. St Louis, USA: Saunders; 2004.
White SD,
Linder KE, Schultheiss P, Scott KV, Page G, Taylor
M, Best SJ, Walder EJ, Rosenkrantz
W, Yager JA. Sebaceous adenitis in four domestic
rabbits (Oryctolagus cuniculus). Vet Dermatol 2000;11:53-60.
|
||||||||||||||||||||||||||||||||||
e-mail: info@medirabbit.com