Hair loss
(alopecia) in rabbits
Esther van Praag, Ph.D.
MediRabbit.com is
funded solely by the generosity of donors.
Every
donation, no matter what the size, is appreciated and will aid in the continuing
research of medical care and health of rabbits.
Thank you
|
Warning: this
file contains pictures that may be distressing for some persons
|
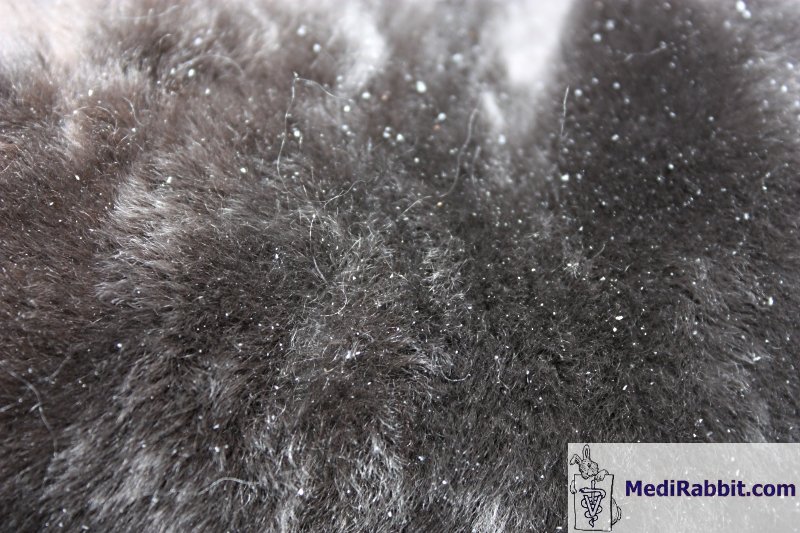
Multifocal alopecia Fur
mite Cheyletiella parasitovorax is most likely to be
found on the dorsum and neck of the rabbit, where it causes dandruff,
seborrheic lesions (lesions from abnormally increased secretion of fatty
matter), and a pruritic (itching) condition. Leporacarus gibbus is found mainly on the dorsum and abdomen. Fur mites can
cause a hypersensitivity reaction. If the condition is severe, alopecia is
observed.
________________________________ Burrowing
mite Wounds appear
first on the lips and nose, later around the head, neck, between toes, and
sometimes around the genitalia. Mange leads to heavy scratching and licking
of the affected region by the rabbit. This leads to alopecia (loss of fur).
Often one can observe the secretion of a watery stuff that forms crusts upon
drying. Self-mutilation will lead to wounds and secondary bacterial
infection.
________________________________ Ear
mite Itching ears, frequent
shaking of the head, and scratching up to the stage of automutilation. In the
beginning, small, tightly adherent skin scales appear deep in the ear canal
and the earlobes and are surrounded by alopecic (balding) regions. Those
yellow-gray scales can be rather thick; they carry large numbers of the
parasite, mite feces, skin cells, and blood. Aside the characteristic lesions on the
ear, the ear mite Psoroptes cuniculi has been observed to infest other
regions of the body, more particularly the ventral abdomen. A. Acar, A. Kurtede, K. Ural, C. Ç. Cingi, M. Ç. Karakurum, B. B. Yagci, B. Sari. Turk. J.
Vet. Anim. Sci. 2007; 31(6): 423-425. An
Ectopic Case of Psoroptes cuniculi Infestation in a Pet Rabbit A
2-year-old female New Zealand rabbit was admitted to Ankara University
Veterinary Faculty, Department of Internal Medicine. Upon physical
examination crustaceous auricular lesions, and erythematous and exudative
pruritic skin lesions, both on the ventral abdomen and on extremities were
detected. Microscopic examination of skin scrapings taken from pinnae and
hair plucked from the ventral abdominal region revealed the presence of
Psoroptes cuniculi. The ventral abdominal localization of P. cuniculi was evaluated
as an ectopic infestation. Despite the injection of ivermectin 0,400 mg/kg
and daily supportive therapy the rabbit died on the fifth day of
hospitalization.
Lesions on the rabbit. a) Inner surface of the pinna; b)
ventralabdomen and extremities. ________________________________ Fleas
and ticks The presence of fleas is
typically subclinical and seasonal. Infestation is characterized by the
presence of the feces of the fleas and their eggs at the periphery of the
ears, between them, on the eyelids or the nose of the rabbit. Other locations
on the body should nevertheless not be ruled out. In rare cases, a strong
allergic reaction against the saliva injected by the flea takes place. The
presence of Spilopsyllus cuniculi often leads to pruritic skin and the
appearance of crusts. Ticks are
usually found while inspecting the fur of a rabbit. Preferred locations are
the ears, the area between the ears, the neck and the dewlap of female
rabbits. Severe infection can lead to macrocytosis. It can be accompanied by
the development of alopecia around the biting site. ________________________________ Bacterial
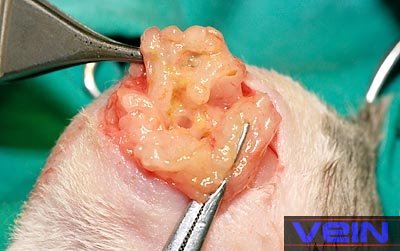
dermatitis or presence of an abscess Abscesses are typically
found on the head, neck and shoulders regions, but can also affect other
parts of the body, organs or bones. During palpation, abscesses
feel either as a hard lump or a soft doughy swelling that can be moved. The
pocket contains a collection of pus, dead phagocytic white blood cells,
necrotic cells, and live or dead bacteria. As the quantity of pus increases,
the pocket grows larger and starts to wall off from the surrounding tissues
and blood circulation. If the abscess is left untreated, it continues to grow
till the tissue will rupture either inside the body or on the surface of the
skin. This stage is particularly painful and dangerous, with the liberation
of bacteria and their toxins in the blood circulation. There are no specific
clinical signs, except the presence of a lump, an unusual swelling, reduced
appetite, increased water intake, or fever. The presence of an abscess is
usually painless, unlike other animals. In case of bacterial dermatitis, the use
of corticosteroid based creams should be avoided; they make the problem worse
the problem.
________________________________ Fungal
dermatitis Typically, lesions start around the head and spread
to the legs and feet, more specifically to the toenail beds. The wound is
raised, circumscribed and erythematous. It shows dry crusts with little or no
pruritus and patchy alopecia. The tissue under the crusts usually shows
inflammation and the hair follicles show abscessation, as the secondary
result of a bacterial invasion. Histological
sections show hyperkeratosis, folliculitis, acanthosis and the diffuse
infiltration of leukocytes into the dermis layer.
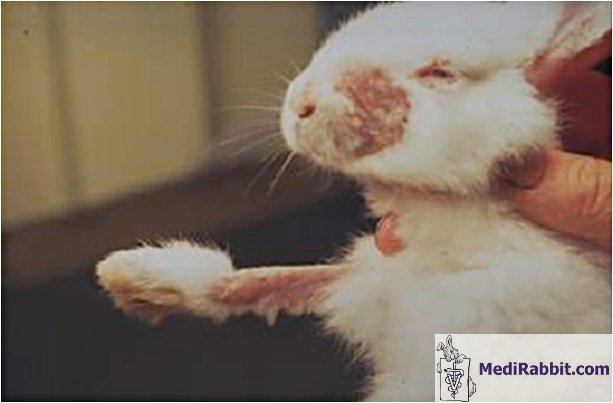
Katleen
Hermans Severe cases of fungal
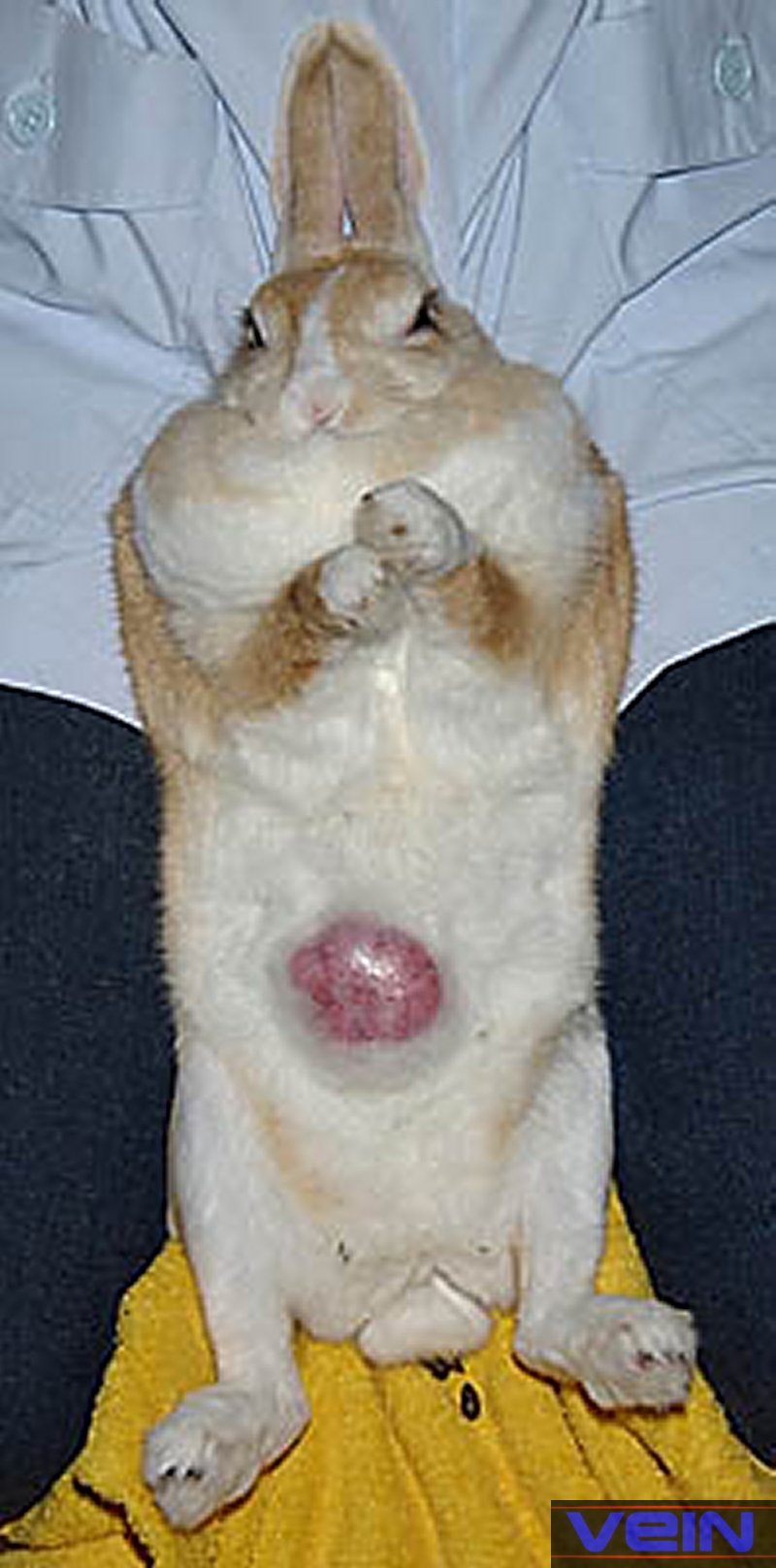
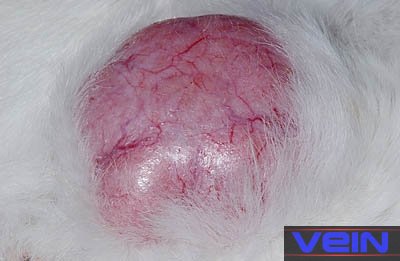
infection on skin, limbs and face ________________________________ Neoplasia, skin
cancer (melanoma, carcinoma, lymphoma)
|
||||||||||||||
|
. |
||||||||||||||
|
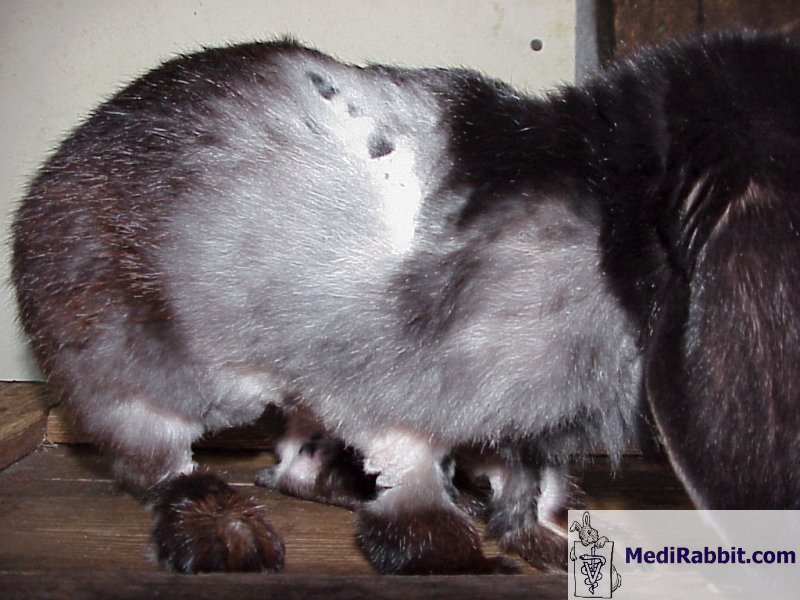
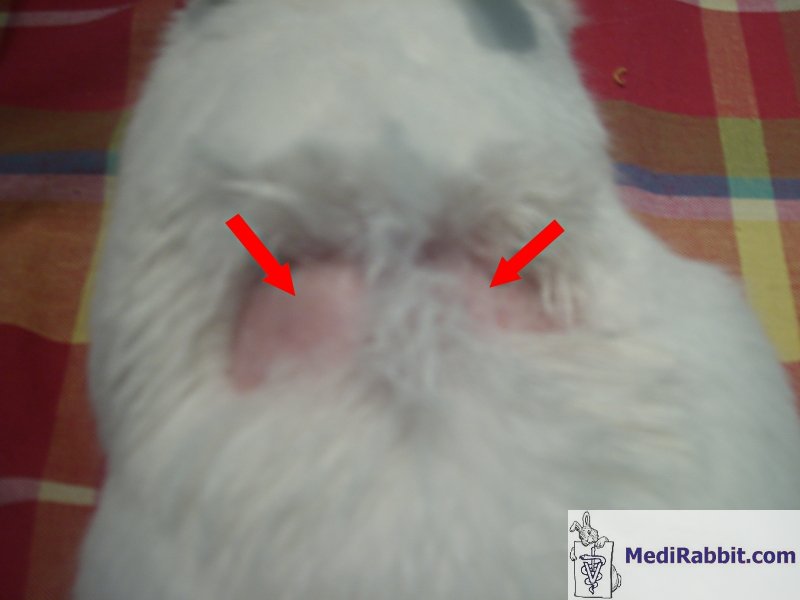
Symmetrical bilateral alopecia Rarely, symmetrical bilateral alopecia is observed
in a rabbit. Due to the scarcity of the cases, and few veterinary
publications on this topic in rabbits, the problem is often misdiagnosed.
Louise Geddes In non-spayed
female rabbits, symmetrical bilateral alopecia may be associated to a hormonal disorder caused
by ovarian diseases. In various animal species, hyperestrogenism is
accompanied by fur thinning in the urogenital region. The mammary glands and
vulva may appear swollen. If radiography does not show the presence of tumors
in other organs or lungs, an emergency ovariohysterectomy may help the rabbit regain health. In one case, symmetrical
bilateral alopecia has
been linked to thymoma, the growth of a benign tumor in the thymus gland,
located in the upper chest. The skin showed features typical of exfoliative
dermatitis and labored breathing. Florizoone K, van
der Luer R, van den Ingh T. Symmetrical alopecia, scaling and hepatitis
in a rabbit. Vet Dermatol. 2007 Jun;18(3):161-4. A 5-year-old rabbit
with inappetence, symmetrical alopecia and skin lesions was examined. No
mites or Malassezia were found in skin scrapings and tape impressions and
dermatophyte culture was negative. Trial therapy with ivermectin did not
reduce skin lesion severity, and euthanasia was performed because of anorexia
after 1 month. Histopathology of the skin showed hyperkeratosis, lymphocytic
exocytosis, cell-poor interface dermatitis (lymphocytic infiltration and
apoptotic cells in basal layer of epidermis), absence of sebaceous glands and
lymphocytic mural folliculitis comparable to sebaceous adenitis and
thymoma-associated exfoliative dermatitis previously described in rabbits.
The liver exhibited an interface hepatitis, comparable to autoimmune
hepatitis in man. The occurrence of morphological similarities to exfoliative
dermatitis and sebaceous adenitis in rabbits, in association with an
autoimmune hepatitis, has not been described before. In some animal species, more so in ferrets,
symmetrical bilateral alopecia has been linked to adrenal disease in
castrated animals. The alopecic skin appeared normal in most seen ferrets.
Adrenal disease is often accompanied by increased sexual behavior and
aggressiveness. In
females, the vulva may appear swollen.
|
||||||||||||||
|
. |
||||||||||||||
|
Congenital alopecia - Hypotrichosis Juvenile
hairlessness is a condition where a young rabbit starts losing fur. It is a
rare condition. The fur either becomes thin, or hair is lost all over the
body, except the tail, the extremities of the limbs, the ears, the nasal
region. Fur may start to grow back after a few weeks. The cause of this
condition is not well understood. If the fur does not regrow with time, the
rabbit may suffer from a mutation that induced the loss of hair, and leads to
so called "furless rabbits". The condition
is related to a mutation that is inherited in a single recessive gene, making
the condition very rare. Hair is rare and limited to guard hair. The skin
shows excessive keratinisation (transformation into a more horny texture of
the outer cells of the epidermis). These rabbit are generally sensitive to
cold temperature. Several variations exist, some rabbits becoming fully
furless, others growing only one type of hair, e.g. only guard hair.
|
||||||||||||||
|
. |
||||||||||||||
|
Behavioral alopecia Pseudopregnancy Female
rabbits that are not spayed can go through cycles of pseudopregnancy. It
usually occurs after the rabbit has been mounted by a castrated male or by a
female rabbit in an attempt to establish dominance, an act which simulates
mating. It is also observed in rabbits living in proximity to a non-castrated
male or in an environment where there are no other rabbits. Hair-pulling is
indicative of the end of pseudopregnancy or pregnancy period. Alopecic spots
may form on the shoulders or abdomen, and may be accompanied by injured and
inflamed skin.
MediRabbit ________________________________ Self-mutilating
behavior Some rabbits engage in
self-mutilation to the point of severe injury to themselves when it includes
chewing the skin down to the bone. Rather than diagnosing self-mutilation as
a psychotic problem, possible causes should be examined and ruled out when a rabbit
shows this behavior. Causes include: ·
Hypersensitive reaction. This involves the immune
system, and is difficult to assess. Such reaction can be triggered by
medication, e.g. intra-muscular injections of ketamine/xylazine can cause skin
irritation, 3 days post-injection. ·
Infestation of the skin by parasites, such as fur
mites, or burrowing mites. ·
Atopy, or hereditary allergic reaction. ·
Frustration in non-castrated female or male
rabbits, driven by hormones to build a nest or find a partner respectively. ·
Contact dermatitis - inflammation of the skin or
rash, caused by contact with an irritating or allergy-causing substance. ·
Neurological
disease. ·
Presence of a foreign body in the fur, e.g. seeds
from grass, oat, burrs or awns (bristle-like appendages found on grasses). Compulsive self-mutilating
behavior has additionally been linked to environmental factors (e.g.
boredom), and to genetic predisposition in specific breeds of rabbits. These
rabbits start to mutilate the pruritic skin of their digits, more commonly in
late summer and autumn (hormonal problem ?).
Histological studies ruled out the presence of skin disease, bacterial,
fungal or parasitic infection, or neurological problems. When genetic
predisposition is determined as the cause, the condition is treated with
psychotic drugs. F. Iglauer, C. Beig, J. Dimigen, S.
Gerold, A. Gocht, A. Seeburg, S. Steier and F. Willmann. Hereditary compulsive
self-mutilating behaviour in laboratory rabbits. Lab Anim
1995;29:385-393 During the last few years an
increasing number of cases of extensive automutilation has
been observed in a rabbit breeding colony of Checkered crosses. Digits and
pads of the front feet were traumatized. No other behavioural abnormalities
or signs of disease were evident. Self-mutilation was seen both in stock,
breeding and experimental animals, in rabbits kept singly in cages and in
those housed in groups on the ground, in rabbits kept in different buildings
and under the care of different staff members. This behavioural abnormality
of Checkered crosses has also been observed in animals after being placed
into other institutions or private homes. No evidence of an agent responsible
for the occurrence of self-injury could be found with parasitological,
mycological, histological, clinical or haematological examination. Twelve to
16 animals are affected yearly in a colony varying in size between 130 and
230 rabbits. Following complete healing,
relapses occurred up to 3 times per year, on either the same or the opposite
front foot. In the last 21 cases episodes of automutilation could be
regularly interrupted with the dopamine antagonist, haloperidol. Similar
signs of automutilation were never seen in animals of another breeding line
kept in the same building and under the same conditions nor in animals
brought in from other breeding colonies. A relatively
high coefficient of inbreeding can be presupposed in this 15-year-old breeding
colony of Checkered crosses. A genetic predisposition for the behavioural
anomaly described appears very likely.
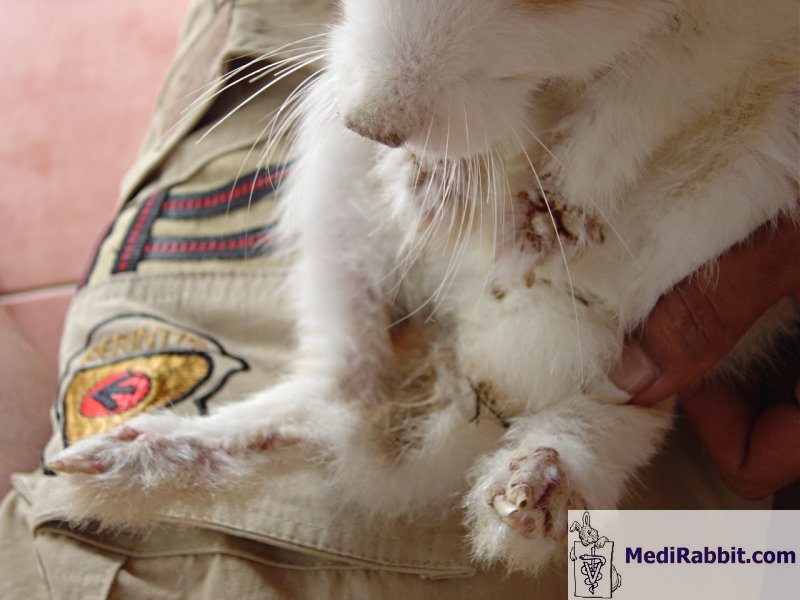
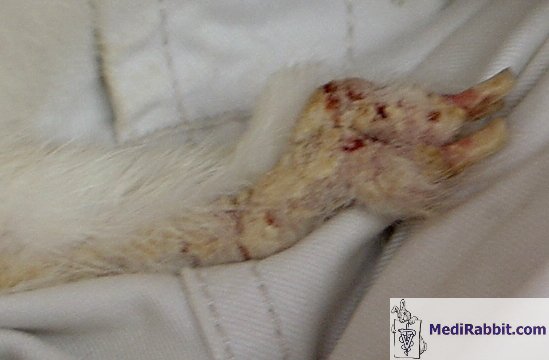
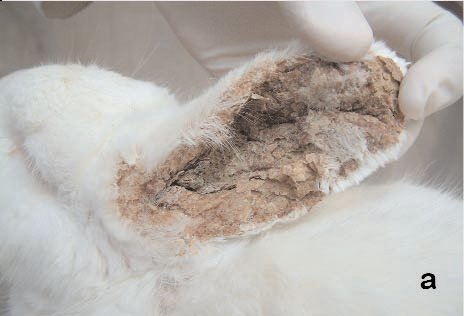
Fig 1A and B Lesions of digits
and pads due to self-mutilation with increasing degrees of severity . |
Many thanks to Ils
Vanderstaey (Belgium), Berend
Bakker (Indonesia), Louise Geddes (USA), Christine Macey (USA), Dr. Kathleen Hermans (Kliniek voor Pluimvee en
Bijzondere Dieren, Universiteit Gent, Belgium), Caroline van Mol (Bunnybunch.nl, Switzerland) and to Akira
Yamanouchi (Veterinary
Exotic Information Network, Japan) for
their help in providing pictures to illustrate this page.
e-mail: info@medirabbit.com