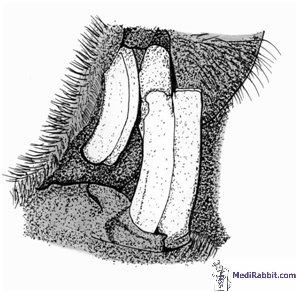
Moist
dermatitis, green fur syndrome, caused by
Pseudomonas
aeruginosa
Esther van
Praag, Ph.D.
|
MediRabbit.com is
funded solely by the generosity of donors. Every
donation, no matter what the size, is appreciated and will aid in the
continuing research of medical care and health of rabbits. Thank you |
|
This skin disorder is caused by bacteria like Staphylococcus
spp., Streptococcus spp., and mainly Pseudomonas aeruginosa.
The later is a Gram-negative, opportunistic pathogen
that lives in aerobic and poor nutritional conditions (the bacterium is able
to grow in distilled water). The bacterium produced 2 pigments, pyoverdin and pyocyanin, when
living in an environment with a low content of iron, which color the hair and
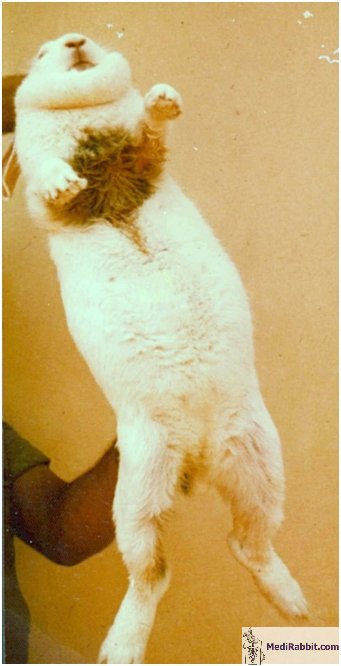
pus oozing out of infected skin or abscesses in a characteristic blue-green. Exudative (relating to the oozing of fluid and other
materials from cells and tissues) moist dermatitis is mainly observed in
rabbits exposed to constant moisture, for instance: • Leaking
water bottles, or inadequate crock; • Overweight; • Large
dewlap (fold of skin which hangs under the throat of female rabbits); • Ptyalism, due to
(severe) dental problems, leading to excessive production of saliva.
Clinical
signs and diagnosis
The clinical
signs should be sufficient for diagnosis. Even so, a bacterial culture is advisable,
as a precautionary measure. The cultures of isolated bacteria will
nevertheless help a proper identification of the bacterium. Sensitivity tests
will furthermore help determine the most efficacious antibiotic. The
bacterium is indeed difficult to treat, as it has naturally acquired
resistance to many antibiotics, while living in the soil, among bacteria,
yeast and fungi that secrete natural antibiotics. Parts of the body affected by
this bacterium are the dewlap, and the abdomen. Lesions are localized and
diffuse and the skin is erythematous and moist. It may be accompanied by the
presence of deep ulcers or abscesses. Secondary bacterial infection is
possible when the condition is left untreated, with the formation of skin
abscesses.
Treatment
The
fur is carefully clipped and the inflamed skin is treated with topical
antibiotics. If the infection by Pseudomonas sp. is severe, the topical
treatment should be accompanied by an aggressive systemic antibiotic therapy.
The
most effective antibiotics remain fluoroquinolone (e.g. enrofloxacin),
gentamycin, and amikacin. Since some strains are resistant to several
antibiotics, a culture accompanied by an antibiotic sensitivity test should
be done. While
treating the skin problems, it is necessary to look for the primary cause of
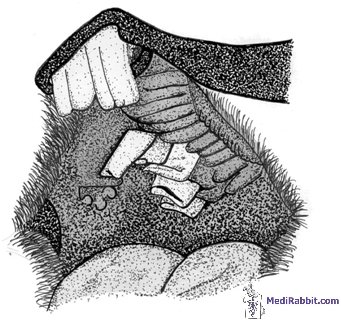
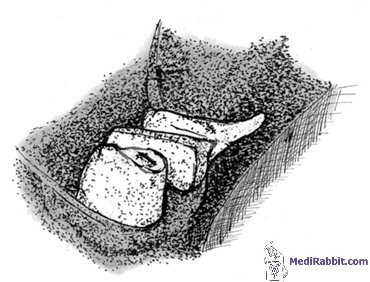
infection. This includes: • Meticulous
inspection of the teeth of the rabbit, in order to detect defects of the
incisors (malocclusion), the presence of spurs or of a tooth root abscess; • Verification
of the drinking habits of the rabbit (crock or water bottle); • Analysis
of the water that the rabbit is drinking for the presence of Pseudomonas
sp. Infections
should not be neglected and left untreated. After the primary invasion of the
skin, Pseudomonas bacteria tend to invade the tissues deeper and will
use the circulatory blood system to disseminate throughout the body.
AcknowledgementThanks are due to Dr. M. Schoenbaum (Ministry of Agriculture, Veterinary Services,
Israel) for the permission to use their pictures. Further information
Garibaldi BA, Fox JG, Musto
DR. Atypical moist dermatitis in rabbits. Lab Anim Sci. 1990 Nov;40(6):652-3. O'Donoghue PN, Whatley BF. Pseudomonas
aeruginosa in rabbit fur. Lab Anim. 1971 Oct;5(2):251-5. Schoenbaum M. Pseudomonas aeruginosa
in rabbit fur. Lab Anim. 1981 Jan;15(1):5.
Wellisch G, Cohen E, Cahane Z, Kedar S,
Fradis M, Podoshin L. Distribution of Pseudomonas aeruginosa serotypes
in Israel. Microbiol Immunol. 1980;24(3):233-35. Williams CS, Gibson RB. Sore dewlap: Pseudomonas aeruginosa
on rabbit fur and skin. Vet Med
Small Anim Clin. 1975 Aug;70(8):954-5. |
e-mail: info@medirabbit.com