Diabetes in rabbits
Esther van
Praag, Ph.D.
|
MediRabbit.com is
funded solely by the generosity of donors. Every
donation, no matter what the size, is appreciated and will aid in the
continuing research of medical care and health of rabbits. Thank you |
|
Diabetes
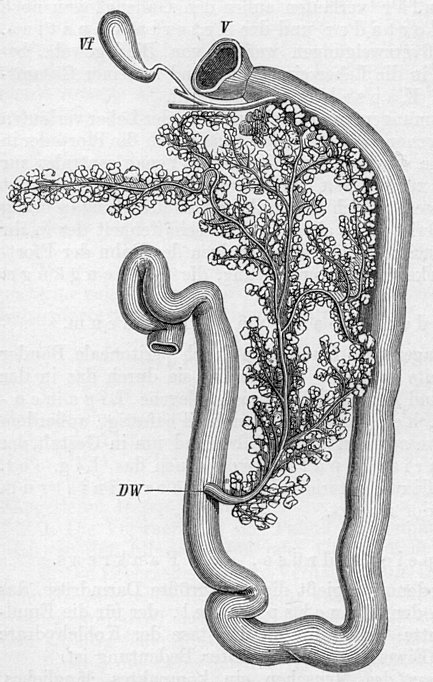
is caused by a dysfunction of the pancreas, an endocrine organ that possesses
islets of Langerhans. Those islets secrete insulin in the blood circulatory system
in order to control the glucose level in the blood and stimulate absorption
of glucose into cells. In experiments where the pancreas of rabbits was
ligated, a strong decrease of insulin secretion (hypoinsulinemia)
was observed, accompanied by an increase of glucagon (hyperglucagonemia).
As a consequence the glucose level in the blood increased considerably.
In human medicine, there are several
types of diabetes: • Type
1
diabetes (or I, or juvenile) and is characterized by a
destruction of the islets of Langerhans. There is still speculation about the
cause: autoimmune, or viral, or viral that triggers an autoimmune reaction
against the virus and the cells of the islets due to mimicry of surface
proteins. An individual suffering from diabetes 1 needs regular injection of
insulin. • Type
2 diabetes is observed mainly in obese persons. Insulin production
remains normal in the beginning, but cells have developed a mechanism of
resistance to the hormone and fail to respond. Consequently the level of
sugar remains high in the blood. An individual suffering from diabetes 2 will
take medication to reduce the level in the blood. True diabetes is a rare to inexistent
condition in rabbits, and is barely described in the literature, with the
exception of obese rabbits and experimentally drug-induced diabetes (e.g., alloxan or streptozotin induced
diabetes). Both type 1, and type 2 have been observed; the symptoms of the
latter being more common in obese rabbits. During the onset phase of the disease,
rabbits were able to compensate for the lack of insulin production in the
pancreas. This led to conclude that insulin may play a less important role in
rabbits and herbivores sugar metabolism, than in carnivores. Many plants have
furthermore hypoglycemic properties and, when ingested, may help the rabbit adjust
its glucose level. A corrected diet, with a great variety of fresh vegetables
and hay would help correct true diabetes or diabetes-like symptoms in a
rabbit, without a need to inject insulin on a daily basis. Clinical signs
In
cases of experimentally induced diabetes, hyperglycemia is accompanied by
polydipsia (excessive thirst), polyuria (excessive urination) and polyphagia
(strong desire to eat). Pathology
In New-Zealand rabbits suffering from type
1 diabetes, endocrine cells of the Langerhans islets were affected and hypergranulation was observed, unlike healthy
non-diabetic rabbits. In other animals, there is usually degranulation. The
lack of insulin production was accompanied by glycosylation of the hemoglobin
(attachment of glucose molecules to hemoglobin, the protein that is involved
in oxygen transport in the red blood cells). When the diabetes was left
untreated, diabetic rabbits suffered the same ill effects than humans:
mineralization of the kidneys, eye trouble and blood vessel problems,
independently from a corrected diet.
DiagnosisManipulation
of a rabbit can lead to an increase of the glucose level in the blood to the order of 8.6 mmol/l and
higher, and will misrepresent the actual level. This phenomenon is triggered by
the release of adrenaline (epinephrine), a molecule that counters the effect
of insulin and enables a raise in the blood glucose. Knudtzon
J. reports about this phenomenon in his papers about diabetes in rabbits. Consequently,
diabetes cannot be diagnosed by one simple blood test; a series of blood and
urine tests must be done over a period of time to confirm the disease. Blood chemistry tests should
include: - blood glucose; - serum osmolarity; - elevated BUN; - electrolytes disbalance
(sodium and potassium); - glucose in urine; - glycosylation of protein (fructosamine
test); - glycosylated hemoglobin
(HbAc1). Hyperglycemia
(overload of glucose in the blood) has been linked to stasis, with poor
prognosis for rabbit; seems to relate to fatty degeneration of the liver. If
the rabbit survives, the glucose level that can be as high as 25 mmol/l, will return to normal. Differential
Diabetes must be differentiated from: •
endocrine disorders, e.g. overproduction of cortisol or glucagon,
Cushing disease; •
disorders of the target organs (liver, fat tissue,
muscle); •
pancreatitis (inflammation of the pancreas); •
renal glycosuria. Treatment
The treatment of choice a healthy diet: •
hay; •
fresh vegetables; •
good quality pellets; •
no "junk" food, treats, rich in
carbohydrates. If the
rabbit is overweight, a weight-reduction plan must be organized. This should
be done slowly, over weeks, rather than days. Insulin injections are not
needed in a rabbit with diabetes. They live well with a healthy diet and no
insulin injections, on the contrary to dogs and cats. Further Information
Catala J, Daumas M, Chanh AP, Lasserre B, Hollande E. Insulin and glucagon impairments
in relation with islet cells morphological modifications following long term
pancreatic duct ligation in the rabbit--a model of non-insulin-dependent
diabetes. Int J Exp
Diabetes Res. 2001; 2(2):101-12. Conaway HH, Faas FH, Smith SD, Sanders LL. Spontaneous
diabetes mellitus in the New Zealand white rabbit: physiologic
characteristics. Metabolism. 1981; 30(1):50-6. Roman-Ramos R, Flores-Saenz JL, Alarcon-Aguilar FJ. Anti-hyperglycemic
effect of some edible plants. J Ethnopharmacol
1995; 48(1):25-32 Roth SI,
Conaway HH, Sanders LL, Casali RE, Boyd AE 3rd.
Spontaneous diabetes mellitus in the New Zealand white rabbit: preliminary
morphologic characterization. Lab Invest. 1980; 42(5):571-9. |
e-mail: info@medirabbit.com