Congestive heart failure in rabbits
Esther van Praag, Ph.D.
|
MediRabbit.com is
funded solely by the generosity of donors. Every
donation, no matter what the size, is appreciated and will aid in the
continuing research of medical care and health of rabbits. Thank you |
The
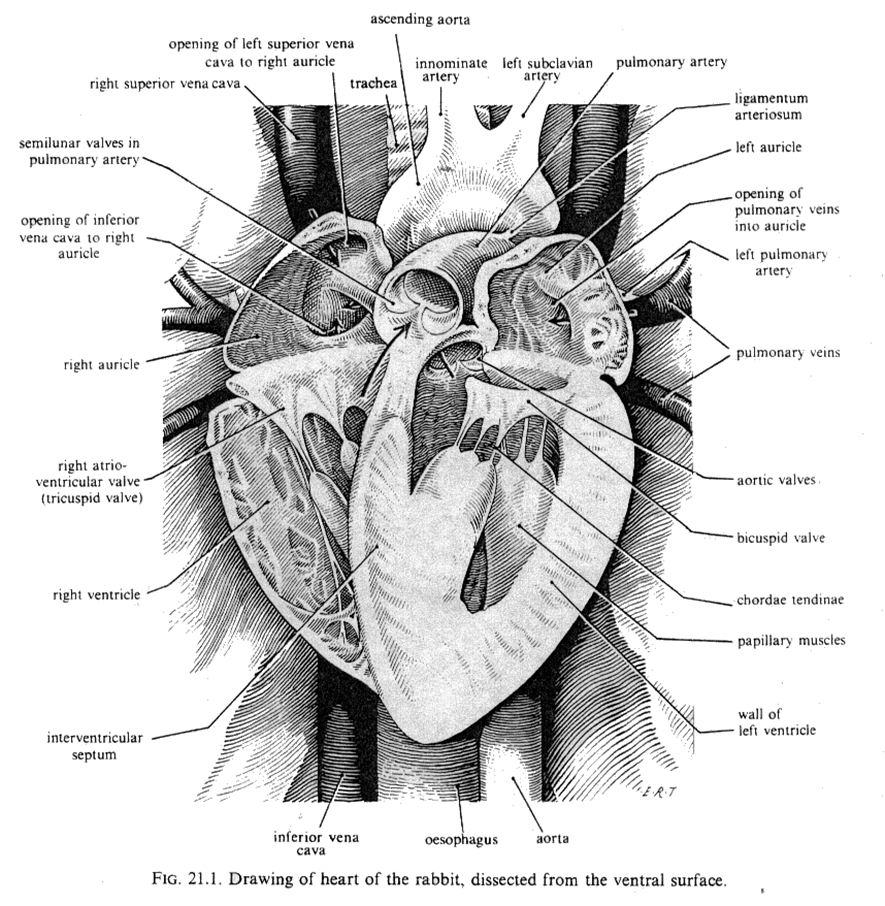
heart is located in the thoracic cavity. Its apex
(the tip of the heart) is directed backwards and slightly to the left, while
its base is directed forwards. The rabbit heart is similar
to the hearts of other small animals in that it is formed by four
chambers: two atria and two ventricles. These chambers are separated by
inter-auricular and inter-ventricular septa. However, the rabbit heart also
possesses some anatomical and physiological particularities.
Atria
are thin-walled chambers that receive blood. In contrast, ventricles are
thick-walled muscular structures that pump blood out of the atrium and back
into the blood system.
In
cases where the left ventricle is unable to expel blood from the left
atrium, or when the mitral valve is malfunctioning, blood accumulation in the
lungs can occur, leading to left-sided heart failure. Congestion of this
nature can lead to pulmonary edema (the accumulation of fluids in the lungs).
Consequently, the body's oxygen uptake and its movement from the lungs to the
heart will be impaired, leading to tiredness. It is frequently accompanied by
labored breathing, also known as dyspnea.
Impaired
right ventricular function or tricuspid valve defects can lead to
elevated blood pressure, resulting in fluid accumulation in body tissues,
particularly in the abdomen and lower extremities.
Causes
The
primary cause of congestive heart failure is a malfunctioning of the left
ventricle. In many cases, this issue is caused by a lack of movement or a
diet deficiency (vitamin and mineral deficiencies) in rabbits. There are
additional factors that contribute to this disorder, including:
·
Arrhythmia
(abnormal heart beat);
·
Bicuspid or
mitral valve defect, either of congenital origin, or caused by an infection
(viral or bacterial), or other diseases;
·
Coronary
disease;
·
Myocardia
related disorders, inflammation or cardiomyopathy;
·
Anemia or low
red blood cell count;
·
Lung diseases,
e.g., pneumonia.
Clinical
signs
Indications
of congestive heart failure may include generalized fatigue and weakness,
anorexia, exercise intolerance, persistent coughing or wheezing and/or
dyspnea.
Various
clinical tests (see: Cardiology
and techniques to detect cardiac diseases in rabbits) often reveal an enlarged heart, increased heart
rate, arrhythmia, and the presence of (lung) edema.
Michel
Gruaz The presence of foam in the nasal cavity
(arrow) in this Belgian bearded rabbit that died suddenly is the sign of a
mixed pulmonary and cardiac distress. . Michel
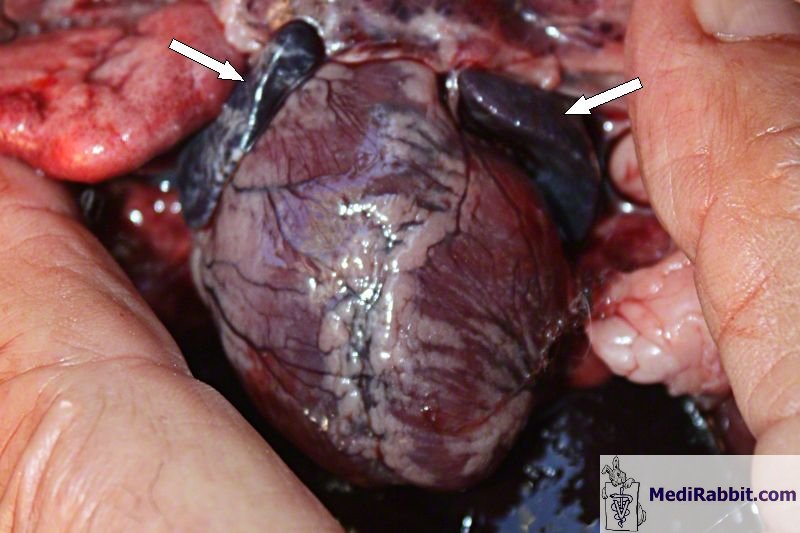
Gruaz During the autopsy, heart of the same
Belgian bearded rabbit, with dark heart auricles (arrows), after a heart
attack and sudden death. Treatment
While
there is no cure for congestive heart failure, treatment can help manage the
condition. The treatment plan includes addressing the underlying disease,
such as pneumonia, with appropriate antibiotics, as well as the
administration of medication to prevent further deterioration of heart
function.
Acute
treatment of congestive heart failure consists of oxygen administration and
rest in a quiet place. The use of diuretics will help relieve the sodium and
fluid retention. Nitrate-based medications (e.g., nitroglycerin) can help
reduce cardiac strain. Therapeutic pleurocentesis
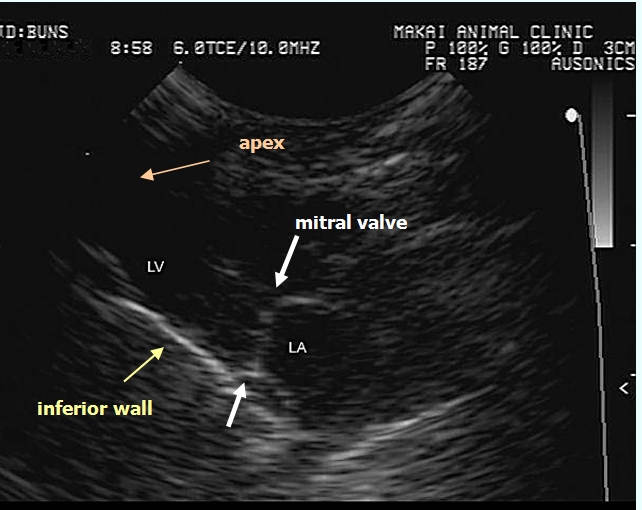
is indicated in rabbits with pleural effusion and severe dyspnea. The
cause(s) should be investigated using echocardiography (ultrasound), for
example.
In
rabbits, long-term management of congestive heart failure includes the use
of:
·
Angiotensin
converting enzyme (ACE) inhibitors such
as enalapril, are medications used to treat high blood pressure. These
medications work by relaxing the blood vessels, which allows blood to flow
more easily. They also reduce the workload on the heart, which can help it to
decrease in size and improve respiration. Enalapril has a slight advantage
over the other available drugs.
·
Diuretics, for example, furosemide is an effective
medication that can help reduce fluid buildup in the body. It increases the
excretion of water and sodium, which can lead to a reduction in the symptoms
associated with heart failure. Dosage is determined by body weight. It can
indeed lead to dehydration and potential kidney failure, while insufficient
intake may not provide the anticipated relief or improvement in symptoms.
Potential side effects of diuretics include low potassium levels in the blood.
·
Inotropic
agents (e.g., digoxin) are used to stimulate a stronger
heartbeat and slightly increase the amount of blood pumped out of the left
ventricle at each contraction. In rabbits, they are used to control sub-acute
and chronic disorders of the myocardium, supraventricular arrhythmia, or
valve regurgitation (leakage of blood from the ventricle back into the atrium
during systole). The use of these medications is contingent upon adequate
monitoring of the hydration status, body weight, appetite, and serum
electrolyte, BUN, and creatinine levels.
Acknowledgement
I would like to express our
gratitude to Tom Chlebecek, DVM (Makai Animal Clinic, Kailua, HI), Frossie Economou, and Michel Gruaz (Switzerland) for
granting me permission to use their pictures on this MediRabbit webpage.
Further
information
M.V. Bray MV, WE. C. Weir EC, D.
G. Brownstein, M. L. Delano, (1992) Endometrial venous aneurysms in three New
Zealand white rabbits. Lab Anim Sci.; 42(4):360-2. Farkas, A. J. Batey, S. J. Coker
(2004) How to measure electrocardiographic QT interval in the anaesthetized
rabbit. J Pharmacol Toxicol
Methods.; 50:175-85. L.C. St John, F. P. Bell (1990)
Arterial fatty acid-binding protein activity associated with
dietarily-induced and spontaneously occurring atherosclerosis in the rabbit (Oryctolagus
cuniculus). Comp Biochem Physiol
B.; 97(1):123-7. C. Kozma, W. Macklin, L. M.
Cummins, R. Mauer (1974) The anatomy, physiology and biochemistry of the
rabbit, in The Biology of the Laboratory Rabbit (Weisbroth
et al., eds), pp 50-69. L. I. Kupferwasser,
M. R. Yeaman, S. M. Shapiro, C. C. Nast, A. S. Bayer (2002) In vitro
susceptibility to thrombin-induced platelet microbicidal protein is
associated with reduced disease progression and complication rates in
experimental Staphylococcus aureus endocarditis: microbiological,
histopathologic, and echocardiographic analyses. Circulation; 105:746-52. C. J. Orcutt (2000) Cardiac and
respiratory disease in rabbits. Proceedings of the British veterinary Zoological
Society (Autumn meeting). K. E. Quesenberry, J. W.
Carpenter, P. Quesenberry (2004) Ferrets, Rabbits and Rodents:
Clinical Medicine and Surgery Includes Sugar Gliders and Hedgehogs, Elsevier
Health, pp 211-216. R. S. Simons (1996) Lung
morphology of cursorial and non-cursorial mammals: lagomorphs as a case study
for a pneumatic stabilization hypothesis. J Morphol. 1996; 230(3):299-316. F.
Harcourt-Brown Textbook of Rabbit Medicine, Oxford, UK:
Butterworth-Heinemann, 2001. |
e-mail: info@medirabbit.com